The focus of the Administration since January 20th has been, appropriately, on COVID. The President’s Relief Bill is expected to pass in the House of Representatives with the Senate’s revisions and could be on the Oval Office desk for signing this week.
Despite problems along the way, we are waiting for the confirmation of Xavier Becerra, Secretary-Elect for the Department of Health and Human Services [HHS]. Chiquita Brooks-LaSure is Joe Biden’s nominee for Administrator of the Centers for Medicare and Medicaid Services [CMS], one of the largest and most important of the 11 divisions within HHS. Both will be critical players in any attempt to expand the Affordable Care Act, addressing health-care equity and access, immigrant health, and other future health care legislative battles.
For now, as the team roster solidifies, I thought it was a good time to republish a Fontenotes from 2017 that many readers found helpful at the time.
A prominent senator kept getting Medicaid and Medicare confused in interviews– he is not the first, nor was he the last. I wrote this guide to help him, his colleagues, and any of you who might be considering public office.
I. Medicare
Memory tip for Senators: “We care for our elderly”
Medicare was passed in 1965 and signed by President Lyndon Johnson. The signing ceremony happened in Independence, Missouri, where President Johnson sat at the table with President Harry Truman, who unsuccessfully fought for insurance for all Americans 20 years earlier. (Truman was not the first President to fight for universal coverage- the idea of a national insurance system can be traced back to Teddy Roosevelt, who was President from 1901 – 1909.)

Medicare was more limited than earlier proposals because it only covered Americans 65 years old and older, but for that population, it had (and continues to have) a dramatic impact. (If that strikes you as a controversial statement, go here.)
Medicare is a Federal program administered by the Centers for Medicare and Medicaid Services [CMS], a part of the Health and Human Services [HHS] Department.
Given the program is run on a country-wide basis, benefits do not differ by region. Medicare for people in Nevada is just like Medicare for people in New Hampshire.
However, the types of coverage an individual may have might vary.
There are four different parts of Medicare:
Part A: This is the basic Medicare package. Everyone gets Medicare A (unless you fall under Medicare C). Medicare A is mainly meant to cover hospital bills but can also include nursing home care (if it involves a nursing/care component), Hospice, and possibly Home Health care. (For more about what Part A covers, go here.)
Part B: Medicare Part B was part of the original law passed in 1965. This part of Medicare is optional- to have it, you need to pay a monthly premium. Medicare Part B covers out-patient care like seeing your doctor at their office, but it also covers the hospital out-patient department, preventive care, drugs given to you at your doctor’s office (as opposed to those you take yourself), physical therapy, and other outpatient services. (For more about Part B, go here.)
[Supplemental Insurance] Although not part of the Medicare plan per se, most Americans with the financial ability to do so purchase Medicare Supplemental insurance from a private company because Medicare Part A and Part B do not cover all expenses a Medicare beneficiary will need.
Part C: This is also known as “Medicare Advantage” or Medicare + Choice.” Part C was created in 1997 under President Bill Clinton to bring private insurance companies into Medicare- both to provide coverage beyond what beneficiaries were getting through Parts A & B (a Part C plan cannot offer less than the standard Medicare package) and to (arguably) lower the cost to the Medicare recipient. This attempt to privatize Medicare remains
Part D: This is the Prescription Drug Benefit passed under President George W. Bush in 2003. The coverage is purchased from private insurance companies to increase the number of Medicare beneficiaries who have insurance to help with drug costs (before Medicare Part D, only about 25% of the elderly had coverage for drugs). A controversial component of Part D is a provision that does not allow Medicare to negotiate lower prices from pharmaceutical companies.
II. Medicaid
Memory tip for Senators: “We offer aid to our poor”
Medicaid passed in 1965 as part of the same law President Johnson signed to create Medicare, but Medicaid is very different than Medicare.
At its core, Medicaid is the program established to offer health care coverage for low-income children, adults, seniors, and those with disabilities. It covers 1 in 5 people in this country, with the majority of funds going to the elderly and disabled, as shown in this graph from the Kaiser Family Foundation:
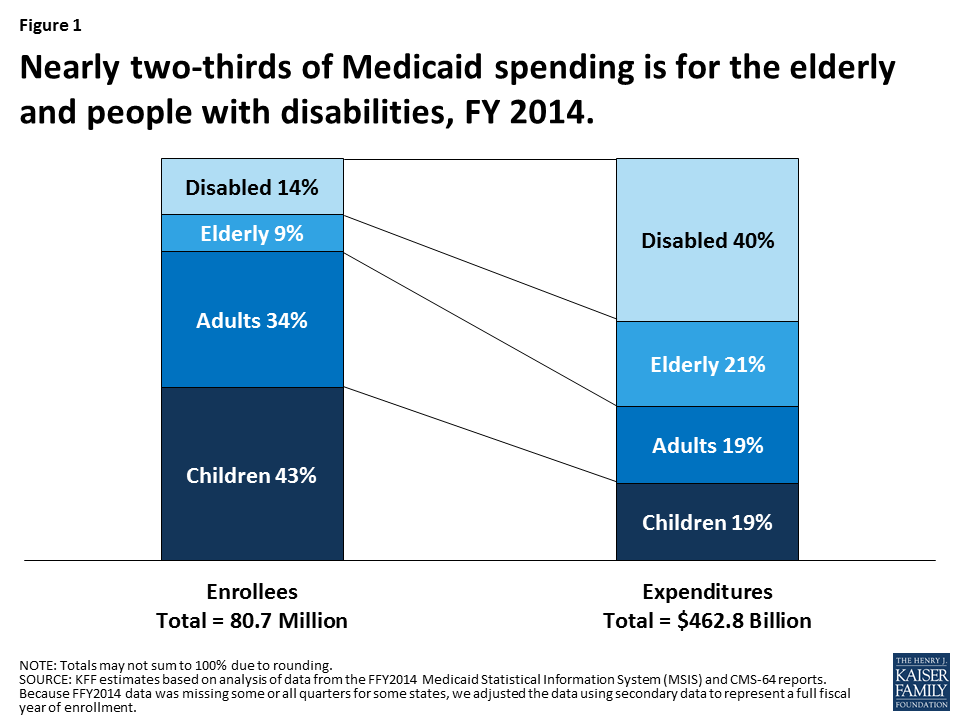
The biggest difference with Medicaid is it is a federal program run by each state. Federal money is given to the states based on actual needs and costs, matching dollar-for-dollar money spent by a state on their Medicaid population.
Because Medicaid is administered by each state, the level of coverage provided, the medical services covered, and the definition of who is eligible all vary significantly (within limits imposed on the federal level).
The ability of a state to control the specifics of their plan explain why “in 2011, Medicaid spending per full-benefit enrollee ranged from $4,010 in Nevada to $11,091 in Massachusetts”. [cite]
The original plan under the Affordable Care Act [ACA or Obamacare] was to expand Medicaid to cover all people below 138% of the federal poverty level (that’s a family of four living on an annual income of $31,000 or less), which also would expand coverage to non-disabled adults- a significant change in many states.
Including all adults on Medicaid would be an enormous difference in several states, such as Texas, where childless adults without disabilities do not qualify for Medicaid between the ages of 18 and 65.)
The ACA plan for expanding Medicaid everywhere was defeated in 2012 by the United States Supreme Court in the pivotal NFIB decision, which held every state had the right to choose whether to expand its Medicaid program under the law.
Initially, 24 states said “No” to Obamacare; the number since that time has dwindled to 19*. (For more on the reasons these states did not participate in expansion and why 32 (including D.C.) went forward with the plan, see Fontenotes # 14.)
That is Medicaid in a nutshell.
*Update for 2021 Readers: The number of states refusing to expand Medicaid is now down to 12. For an explanation and interactive map, go here.)
Which Costs More?
This summer, as the GOP-controlled Senate and House of Representatives could not “Repeal & Replace ObamaCare,” most of the debate was over conflicting opinions on what to do with Medicaid. Curtailed spending, increasing a state’s ability to dictate the terms of their Medicaid program, and “block grants” were all part of the (ultimately unsuccessful) arguments.
With all the focus on cost, it would be easy to assume that it is Medicaid that is draining our federal coffers – so I will leave you with one more graph (and please note it is Social Security- which we all get- that is the heftiest social program in the pie!)
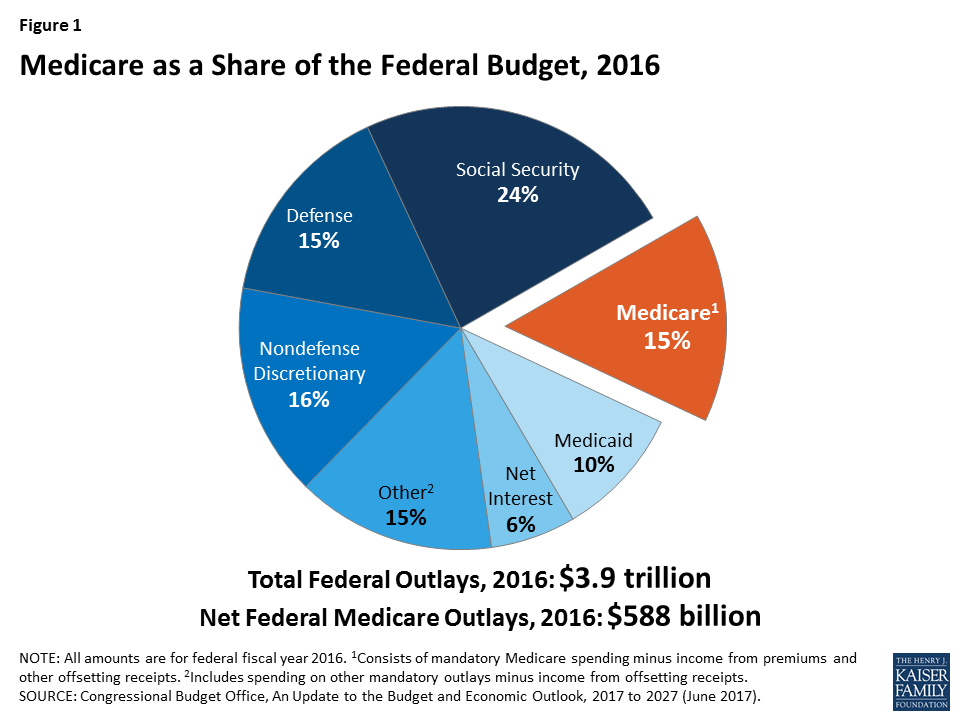
That ends a quick tutorial on two enormously complex programs.
I hope you are now ready to speak on a Sunday Morning news program without embarrassing yourself!
Want to know more?
- Here is a fun timeline from Kaiser Family Foundation where you can peruse what was happening in American healthcare in 5-year increments, all the way back to the early 1900s.
- You might also be interested in this article which addresses whether medicine before Medicare was “the Golden Years” in American health care.